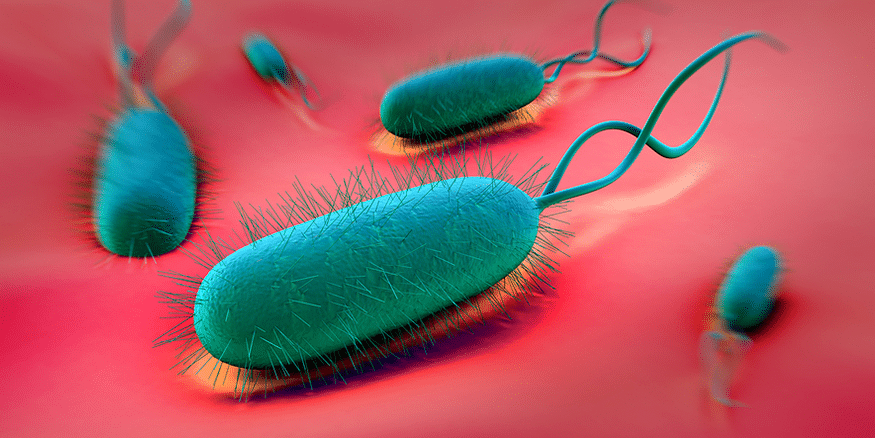
H. pylori: More than Gastric Ulcers
The scientific community used to believe that stress caused gastric ulcers. It wasn’t until 1982, when two scientists, Dr. Barry J. Marshall and Dr. J. Robin Warren, discovered that a bacterium that lives in the gut, Helicobacter pylori, is the real cause of most gastric ulcers. They would later receive the 2005 Nobel Prize for Physiology or Medicine for this important discovery. Around half the population is infected with H. pylori, which they typically contract in childhood,1 but many of these individuals do not develop ulcers, and the scientific community is not sure why. Recently, researchers have been conducting more research into this newly discovered bacterium, to see what other effects it may have in the human body.
Could treating H. pylori be a risk factor for obesity?
Previously, we discussed the impact that gut bacteria can have on your weight and the amount of body fat you carry. In further support of this, a recent study analyzed the possible impact of H. pylori on the population’s propensity toward obesity.2 The study authors found that in populations where H. pylori infection was most prominent, people tended to be thin, and in cultures where H. pylori eradication is common, the obesity rates were very high.
The researchers ran a meta-analysis, combining data from 49 studies from 10 European countries, Japan, the US, and Australia that had information on H. pylori rates and obesity.
In some of the studies they looked at, researchers compared weight gain in individuals being treated for H. pylori to weight gain in those who received placebo treatment, and found significant weight gain in patients upon treatment of H. pylori that was not present in those who received the placebo treatment.
In addition, animal studies showed that H. pylori infection suppressed weight gain, decreased fasting blood glucose levels, improved glucose tolerance, and increased levels of leptin (a hormone that causes you to feel full).
However, this tendency toward lower weight is also harmful for some individuals: children who were never infected, or those who cleared the infection, grow faster than those with persistent H. pylori.
The researchers are unsure why this correlation exists, and more studies need to be conducted to really understand, but it does seem clear that our unique microbiomes have more effects on our bodies than we realize.
Inverse Correlation between H. pylori and IBD
Previous research has provided some evidence of an inverse relationship between infection with H. pylori and inflammatory bowel disease (IBD), meaning that lack of this bacterium in the body seems to relate to a greater risk of IBD.
In a large study from Texas, researchers compared 1,061 IBD patients with 64,451 non-IBD control participants.3 Individuals in the control group were twice as likely to harbour H. pylori infection. In addition, the study showed that IBD patients who experience gastritis (inflammation of the stomach), which is commonly associated with H. pylori infection in healthy individuals, are much less likely to be infected with H. pylori than non-IBD patients with gastritis. Future research could determine the full nature of this inverse relationship with H. pylori and of the particular microbial balance present in the gut of IBD patients when they experience gastritis without H. pylori infection. The researchers say that understanding this relationship would bring them much closer to understanding the development (pathogenesis) of IBD.
